Molecular characterization of lung squamous cell carcinoma tumors reveals therapeutically relevant alterations
Joshi A, Mishra R, Desai S, Chandrani P, Kore H, Sunder R, Hait S, Iyer P, Trivedi V, Choughule A, Noronha V, Joshi A, Patil V, Menon N, Kumar R, Prabhash K, Dutt A.Unlike lung adenocarcinoma patients, there is no FDA-approved targeted-therapy likely to benefit lung squamous cell carcinoma patients. Moreover, most of the reported studies describe Caucasian, Chinese, Korean and Japanese population, with sparse information on the molecular profile of lung squamous patients of Indian origin that accounts for about 30% of Indian lung cancer disease. We earlier reported the first landscape of actionable alterations in lung adenocarcinoma patients of Indian origin (Ann Oncol. 2017 Mar 1;28(3):597-603). Here, we present the first genetic landscape of alterations underlying 430 Indian lung squamous genomes and uncover the prevalence of known targetable somatic alterations using next generation sequencing followed by validation using mass spectrometry. Specifically, we perform whole exome sequencing followed by mass spectrometry-based genotyping of 430 tumors using a customized panel of 53 hotspot mutations across 17 genes, along with detailed clinical correlation survival analyses of the patients harboring the alterations.
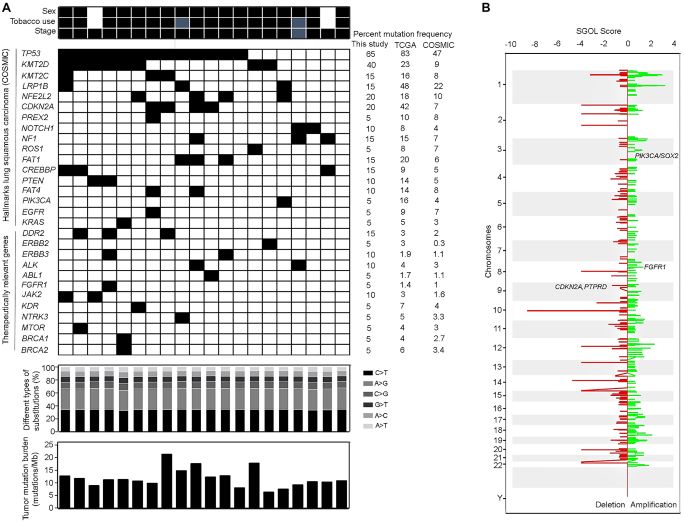
Our study reveals 19% lung squamous patients harbor mutations across TP53, CDKN2A, FGFR1, PTEN, KMT2C, LRP1B, FAT1, NFE2L2 and PREX2. Of these, 13.5% of lung squamous tumors harbor mutually exclusive oncogenic mutations in KRAS, FGFR2, NRAS and ERBB3. Among therapeutically relevant frequent oncogenic mutations EGFR-tyrosine kinase inhibitor sensitive alterations were observed at a frequency of 5.8% in our cohort, significantly higher than as reported in the TCGA and other studies; KMT2D mutations were observed at a frequency of 40% compared to 10% and 24% compared to the Caucasian and East Asian population; and, 10.5% alterations in the PI3K-AKT pathway. Interestingly patients harboring druggable oncogenic mutations showed lower median overall survival (165 days) compared to patients harboring other mutations, (221 days). Similarly, 19% lung squamous patients harboring a mutation in at least one gene resulted in a statistically significant shorter median overall survival compared to lung squamous patients with (167 days vs 225 days). These mutations could help inform designing a panel of specific and actionable mutations to select lung squamous patients likely to benefit from personalized treatment and follow up diagnosis based on liquid biopsy for disease progression and recurrence as shown for lung adenocarcinoma.
In summary, we present in-depth profiling of genetic variations prevalent in Indian lung squamous tumors and identify EGFR and PIK3CA as druggable targets and potential biomarkers in 16.5% patients, which could further extend the scope of ongoing clinical trials and guide in treatment decisions.